Sleep is essential to good health and good mental function, but many Americans struggle to get the rest they need. Approximately 40 million people in the United States suffer from sleep disorders, with the prevalence evenly spread between men and women. Although both sexes are equally likely to have disordered sleep, there are differences in the types of sleep disorders men and women suffer from. Researchers in chronobiology may have discovered the cause of this difference: The influence of sex hormones on the circadian rhythm.
How Men and Women Sleep
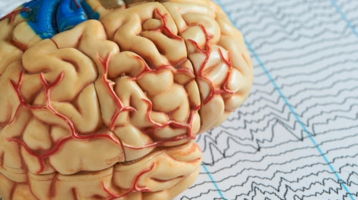
 All healthy people follow the same basic cycle when they sleep, going through several phases and cycling in and out of REM sleep. These cycles are carefully timed by the brain to allow important physiological processes such as cell repair to occur. A lack of good sleep has been linked to serious health problems such as heart disease, diabetes and even cancer.
All healthy people follow the same basic cycle when they sleep, going through several phases and cycling in and out of REM sleep. These cycles are carefully timed by the brain to allow important physiological processes such as cell repair to occur. A lack of good sleep has been linked to serious health problems such as heart disease, diabetes and even cancer.
However, for people with sleep disorders, getting the sleep needed to maintain good health and function is a challenge. There are two types of sleep disorders: central and obstructive. Central sleep disorders are caused by innate biochemical issues in the body, such as low melatonin levels, while obstructive sleep disorders are caused by obstruction of the respiratory tract that prevents good rest.
Gender Differences in Sleep Disorders
While men and women have similar sleep needs and similar risk of sleep disorders, the type of sleep disorders they are prone to varies between the sexes. Men are more prone to obstructive sleep disorders, especially sleep apnea. Women, on the other hand, tend to have central sleep disorders, usually ones affecting the ability to fall asleep at a reasonable time and stay asleep. Common conditions of the female body such as pregnancy and polycystic ovarian syndrome may cause sleep disorders.
New research is offering insight into this gender difference. First, researchers suggest that women may have different symptoms of apnea and thus not be as likely to be diagnosed. Second, sex hormones and natural hormonal cycles may be responsible for the differences.
The Princess and the Pea?

During menopause, a woman’s natural hormonal cycles become irregular and then menstruation ceases altogether. Unsurprisingly, this is a time when sleep is more likely to become disordered. Around half of all menopausal women report sleep disturbances, especially insomnia. Sleep studies have found these women also have less REM sleep than is ideal. Researchers in circadian biology believe that estrogen and progesterone both support healthy sleep cycles in moderate amounts, but that fluctuations in these female hormones can make it difficult both to fall and remain asleep.
Male Sex Hormones and Sleep

In particular, testosterone appears to be linked to sleep. Testosterone levels rise during REM sleep and then fall during the day. People who do not get enough REM sleep because of obstructive sleep apnea, for example, may then suffer low testosterone and the many symptoms associated with it. Men with obstructive sleep apnea are more likely to have low testosterone as well, supporting this hypothesis.
The influence of gonadal (or sex) hormones on sleep remains a hot area of study in chronobiology. Hormonal changes clearly have an effect on sleep, and sleep quality may in turn affect hormone levels. Figuring out the precise link between sex hormones and sleep may allow many people to have their sleep disorders treated and finally get the good night of rest that they need.