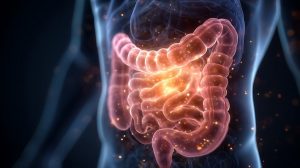
For more than 100 years, scientists have been pursuing the idea of insulin in tablet form, often referred to as the “dream therapy” for diabetes. The challenge lay within the body itself. Enzymes in the digestive system break down the insulin before it can take effect, and the intestines lack a natural way to absorb it into the bloodstream. As a result, many patients still rely on daily injections, which can impair their quality of life. A team at Kumamoto University led by Associate Professor Shingo Ito has now developed a promising solution. Their approach utilizes a cyclic peptide capable of passing through the small intestine, known as the DNP peptide. This platform enables the oral administration of insulin in a way that was previously impossible.
Two Effective Strategies for Intestinal Absorption
To achieve this, the researchers developed two different methods designed to help insulin overcome the intestinal barrier:
1. Blending method (interaction-based): The team combined a modified “D-DNP-V peptide” with zinc-stabilized insulin hexamers. When administered orally to various diabetes models, including chemically induced (STZ mice) and genetic (Kuma mice) models, this mixture rapidly lowered blood glucose levels to normal. Stable blood sugar control was maintained with once-daily dosing over three consecutive days.
- DNP peptide: The cyclic peptide can cross the intestinal barrier. It temporarily binds to the insulin complexes, thereby facilitating their passage through the intestinal wall into the bloodstream.
- Advantage: The insulin molecules are effectively transported into the bloodstream without the need to chemically modify each individual unit.
- Results in animal models: In mice with type 1 diabetes (chemically induced or genetic), blood sugar normalized rapidly, and a single daily dose was sufficient to maintain stable blood sugar control over three days.
2. Conjugation method (covalent): Using click chemistry, the researchers bound the DNP peptide directly to insulin, thereby creating a “DNP-insulin conjugate.” This version lowered blood sugar just as effectively as the mixing method, confirming that the peptide actively helps transport insulin through the intestine.
- Direct binding: The peptide is now firmly coupled to the insulin, allowing both molecules to be transported through the intestine as a single unit.
- Mechanism: The DNP peptide continues to act as a “key” for the intestinal barrier, but now pulls the insulin directly into the bloodstream with it.
- Advantage: Higher absorption efficiency, as each insulin molecule reliably utilizes the transport mechanism.
- Results in animal models: The DNP-insulin conjugate lowered blood sugar just as effectively as the mixing method, but confirmed that direct coupling allows for even more targeted use of the peptide.
Lower Doses Make Oral Insulin More Practical
One of the biggest obstacles to oral insulin has been the need for extremely high doses—sometimes more than ten times higher than with injections—because much of the insulin was broken down by enzymes in the gastrointestinal tract or failed to enter the bloodstream effectively. This made oral insulin preparations impractical and expensive and increased the risk of unwanted side effects. This new platform significantly reduces this requirement. It achieved a pharmacological bioavailability of approximately 33–41% compared to subcutaneous injection. This efficiency suggests that oral insulin could become far more practical for everyday use. Patients would no longer need to take extremely high doses, which simplifies daily administration and increases acceptance. Lower doses reduce the risk of unexpected hypoglycemia and minimize potential strain on the digestive tract. Less insulin per dose also means a more cost-effective therapy, which is particularly crucial for long-term, daily use. Even with once-daily administration over several days, blood sugar levels in the animal model were effectively normalized, indicating reliable efficacy.
The Role of Chronobiology
Chronobiology, the science of biological rhythms, plays an increasingly important role in the efficacy of insulin, particularly in the context of new oral administration methods. Our metabolism is subject to natural daily rhythms: Blood sugar levels fluctuate not only in response to meals but also throughout the day—for example, in the morning after waking up, during periods of activity in the daytime, and at night during sleep. At the same time, the activity of digestive enzymes, the permeability of the intestinal wall, and the absorption of nutrients change throughout the day, which has a direct impact on how and when insulin becomes effective in the blood. Traditional insulin injections can only account for these circadian fluctuations to a limited extent, which often leads to under- or overdoses and makes blood sugar control difficult.
New technologies, such as oral insulin delivery based on DNP peptides, open up entirely new possibilities here. They could be designed so that insulin is available in the bloodstream precisely at the times when the body needs it most—for example, before meals or during periods of increased glucose production by the liver. By taking these natural biological rhythms into account, such formulations not only enable more stable blood sugar control but also allow for individualized treatment. This means that patients receive an insulin supply that harmoniously integrates into their daily routine and the body’s physiological processes, thereby improving quality of life and reducing the risks of blood sugar spikes or drops. Ultimately, this demonstrates how the combination of chronobiology and modern insulin technology can create a new approach to personalized diabetes treatment that goes beyond mere blood sugar control and respects the body’s natural rhythm.
Future Potential for Diabetes Treatment
“Insulin injections remain a daily burden for many patients,” said Associate Professor Shingo Ito. For many people with type 1 diabetes, each injection means not only physical pain but also psychological stress and a limitation in daily life. “Our peptide-based platform offers a new route for the oral administration of insulin and could be applicable to long-acting insulin formulations and other injectable biologics.” This concept could significantly improve patients’ quality of life, as it eliminates the daily routine of injections and allows insulin intake to be better aligned with natural blood sugar and metabolic rhythms.
In the long term, such developments could fundamentally transform diabetes treatment: less burden from injections, more stable blood sugar levels, reduced risks of hypoglycemia and hyperglycemia, and better adaptation to individual lifestyles and daily rhythms. At the same time, the platform opens the door to further innovations in the oral administration of complex medications, which could be of enormous significance not only for diabetes but for many other chronic diseases. The results were published in the journal Molecular Pharmaceutics. The researchers are now conducting further studies, including tests on larger animal models and systems that mimic the human gut, as they work toward future clinical application.