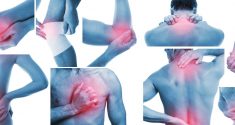
Treating high blood pressure and cardiovascular disease can be a challenge for modern physicians. Unfortunately, the stakes are high. 720,000 people in the United States have heart attacks every year, while 60 million have some form of cardiovascular disease. Controlling blood pressure is very important in maintaining a healthy cardiovascular system while preventing heart attack and stroke.
While new wonder drugs for hypertension hit the pharmaceutical market almost every year, many people still live with uncontrollably high blood pressure and the accompanying high risk of heart attack. However, new studies in chronobiology show that chronotherapy, or timing therapies and medication according to the circadian rhythm, may present a hopeful new avenue of treatment.
The Internal Clock of Cardiovascular Function
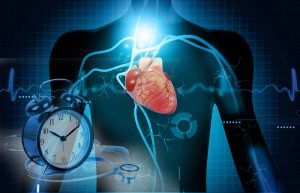
Blood pressure increases further in the morning when a person rises and begins moving. This increases demands on the heart, which must begin pumping more blood to maintain oxygen supply to the body. Platelets are also more likely to form clots in the morning, increasing the risk of stroke and other cardiovascular events.
After peaking in the morning, blood pressure declines throughout the day and reaches its 24-hour low between midnight and 3 a.m. The pulse follows the same basic rhythm. Researchers believe that both blood pressure and heart rate are governed to a large degree by sympathetic tone, a biological system which acts through hormones such as epinephrine and norepinephrine. Sympathetic tone is higher during the day to keep the body and mind alert and ready for activity.
Dippers and Nondippers
When studying the rhythmicity of heart attacks and blood pressure, circadian biology researchers quickly realized that their patients followed one of two daily patterns. These two groups of patients were called dippers and nondippers. Dippers have a night blood pressure that is at least 10 percent less than their daytime blood pressure, while nondippers show a much smaller dip. This is significant because nondippers have a greater risk of death from a cardiovascular event, suggesting that a normal circadian rhythm is important to heart health and disease prevention. Nondippers are at an especially high risk of nighttime heart attack.
Chronotherapy: Applying New Knowledge

Calcium channel blockers, another common medication for hypertension, show decreased bioavailability when given in the evening. Despite this, certain drugs in this class are helpful with nighttime blood pressure in nondippers. Two drugs even convert nondippers back to the normal blood pressure rhythm of a dipper, which may reduce the chances of sudden death.
ACE inhibitors are taken once a day, but people who are nondippers see a drastic lowering of blood pressure when they take them at night rather than in the morning. Timing this drug correctly may prevent many of the late night heart attacks seen in nondippers.
A person’s circadian rhythm, including whether they are a dipper or nondipper, can make a huge different in what treatments and timing are the most effective. Many lives may be saved by simple testing to determine how a patient’s blood pressure changes at night and then applying chronotherapy according to their type. These new findings offer hope for people who struggle to control hypertension as well as the medical team trying to help them.