Research led by Dr. Christine Swanson, MCR, examined whether getting enough sleep can help prevent osteoporosis. “Osteoporosis can occur for many reasons, such as hormonal changes, aging, and lifestyle factors,” said Swanson, an associate professor in the Department of Endocrinology, Metabolism, and Diabetes. “But for some of my patients, there is no explanation for their osteoporosis. That’s why it’s important to look for new risk factors and consider what else changes over the course of a lifetime, just like bones—sleep is one of them.”
What is Osteoporosis?
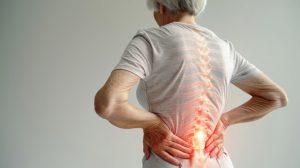
How Bone Density and Sleep Change Over Time
In their early to mid-20s, people reach what is known as peak bone mineral density, which is higher on average in men than in women, as Swanson explains. This peak value represents a crucial “bone reserve” and is one of the most important factors for future fracture risk. It is not only genetically determined but is also influenced by diet (particularly calcium and vitamin D intake), physical activity, and hormonal factors. Once this peak is reached, bone density remains relatively stable for several decades, as long as the balance between bone formation and resorption is maintained. With increasing age, however, this balance gradually shifts in favor of bone resorption. In women, the decline in estrogen during menopause leads to a particularly rapid loss of bone mass, as this hormone has a protective effect on bone metabolism. But bone density also decreases continuously with age in men, albeit usually more slowly, due in part to falling testosterone levels and age-related changes in metabolism.
Sleep patterns also change significantly over the course of a lifetime. With increasing age, total sleep duration tends to decrease, and the structure of sleep shifts—for example, it often takes longer to fall asleep, and nighttime awakenings occur more frequently. At the same time, the proportion of slow-wave sleep—the deep, particularly restorative sleep—decreases, while lighter sleep phases dominate. These changes can affect important regenerative processes in the body, including hormonal regulation such as the release of growth hormone, which plays a role in bone formation. Additionally, sleep often becomes more fragmented and less efficient with age, which can further impair the quality of rest.
“And it’s not just sleep duration and sleep composition that change. Circadian phase preference also shifts over the course of a lifetime in both men and women,” said Swanson, referring to individual preferences for sleep and wake times. Younger people often have a later internal clock (“evening type”), while older adults tend to get tired earlier and wake up earlier (“morning type”). This shift in the internal clock is accompanied by changes in the release of hormones such as melatonin and cortisol, which regulate the sleep-wake cycle. In addition, as we age, the circadian system becomes more sensitive to external influences such as light or irregular daily routines. These changes can lead to less stable sleep and biological rhythms, which in turn can affect various physiological processes—including bone metabolism.
How is Sleep Related to Our Bone Health?
Genes that control our internal clock are active in all bone cells, where they regulate fundamental processes of bone metabolism. When these cells break down and rebuild bone, they release specific substances into the blood—so-called markers of bone resorption and formation—which can be used to estimate current bone turnover. These markers follow a distinct daily rhythm controlled by the circadian clock. It is notable that the fluctuations (amplitude) in markers for bone resorption—that is, bone breakdown—are more pronounced than those for bone formation. This means that the breakdown process is subject to greater biological fluctuations throughout the day and could be particularly sensitive to disruptions, such as sleep deprivation, shift work, or irregular sleep schedules.
This rhythm is likely crucial for healthy bone metabolism. If disrupted, the balance between bone formation and resorption can be thrown off, which could lead in the long term to reduced bone density and an increased risk of diseases such as osteoporosis. The close connection between sleep, the internal clock, and bone metabolism suggests that circadian disruptions directly influence bone health. Therefore, it is becoming increasingly important to view sleep not only as a restorative factor but also as a potential risk factor for bone health—especially since both sleep patterns and bone structure change significantly over the course of a lifetime.
Investigating the Link Between Sleep and Bone Health
The research team measured markers of bone turnover at the beginning and end of this intervention and found significant adverse changes in bone turnover in both men and women in response to the sleep and circadian disruption. The adverse changes included a decline in markers of bone formation, which was significantly greater in younger individuals of both genders compared to older individuals. In addition, young women showed a significant increase in the marker for bone resorption.
If a person forms less bone while continuing to resorb the same amount—or even more—this could lead to bone loss, osteoporosis, and an increased risk of fractures over time, according to Swanson. And gender and age may play an important role, with younger women potentially being the most vulnerable to the adverse effects of poor sleep on bone health. While research in this area is still in its early stages, it is increasingly providing evidence that sleep quality and circadian stability are previously underestimated but potentially critical factors for long-term bone health.