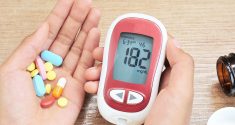
While the immune system is vital to everyone’s continued health, it plays an especially important role in people with Type 2 diabetes. This is because a simple injury can turn into a life-threatening complication unless the body heals that wound efficiently. When an individual develops Type 2 diabetes, the body can’t produce sufficient levels of insulin. Lower levels of insulin in the body mean that glucose isn’t properly regulated, which raises the body’s blood sugar levels. In turn, a higher level of blood sugar inhibits the immune system’s ability to heal wounds.
Wounds that take a long time to heal can develop ulcers, which are open sores that don’t receive sufficient blood circulation. This type of ulcer is most common on the feet of diabetics and can result from even minor foot wounds. The American Podiatric Medical Association reports that as many as 24 percent of people with foot ulcers must eventually have the limb amputated. The seriousness of a foot wound for people with diabetes compels them to seek medical treatment for minor injuries, as a means of reducing the chances that an amputation will be necessary.
How Common are Diabetic Ulcers?
Diabetic ulcers are more common than people realize, with 15 percent of diabetics developing chronic wounds, and ultimately ulcers. Of all people who develop chronic wounds, ulcers develop in about 1.5 million cases. This contributes to a 15-times higher risk of limb amputations in those with diabetes.
As a result of slower wound healing and the development of ulcers, over 60,000 diabetics undergo limb amputations each year. Even where an injury doesn’t occur, neuropathy, or the loss of feeling, can lead to the same results. Once neuropathy begins to develop, the individual is more likely to develop injuries and sores, chronic infections and gangrene. Any of these conditions significantly increase the likelihood of an amputation. The American Diabetes Association believes the need for amputations would be reduced by half if patients with diabetes were educated and routinely tested for neuropathy.
The concern over the high number of amputations has led researchers to study how diabetes affects the immune system. The latest studies indicate that poor sleep slows wound healing, suggesting that the immune system is compromised by insufficient amounts of quality sleep.
Study Confirms That Poor Sleep Slows Wound Healing

A study led by the University of Tennessee at Knoxville professors Mark McLain and Ralph Lydic and recently published in the journal SLEEP linked poor sleep to inhibited wound healing. To study the effects of sleep on wound healing, researchers selected a sampling of 34 mice and divided the rodents into two groups. The test group consisted of obese mice with Type 2 diabetes, while the second group was made up of mice with healthy weights and that did not have diabetes. After anesthetizing the mice, a small incision was made on the back of each mouse. Some mice were then permitted a normal sleep schedule, while other mice had their sleep patterns interrupted at irregular intervals.
The researchers found that those mice with diabetes, whose sleep patterns were interrupted experienced a slower healing cycle than the other rodents. The mice who experienced poor sleep patterns took 13 days to reach a point at which their wounds were 50 percent healed. The other mice healed at a faster rate, reaching the 50 percent benchmark by the tenth day.
The mice in the second group, which consisted of healthier animals without Type 2 diabetes, healed the fastest. They reached the 50 percent mark within just one week and were completely healed by the end of the second week.
Can a Good Night’s Sleep Boost Immune Health?
This latest research indicates that poor sleep quality can actually increase the likelihood of infection. By inhibiting the immune system and slowing down the healing process, the opportunity for contracting an infection is increased. In people with diabetes, any infection can lead to an ulcer and the necessity of amputation.
Just as poor sleep slows wound healing, Professor Lydic hopes the opposite may be true and improved sleep can strengthen the immune system. He plans to conduct more research in this area, which may ultimately lead to new treatments for diabetes. Next, the researcher is interested to see how certain drugs affect the healing of wounds when the sleep pattern is interrupted. The research may ultimately lead to a way of boosting immune system functioning for people with Type 2 diabetes.
Diabetes is a growing problem in the United States. Even prediabetes, a condition in which blood sugar levels are just below the threshold for a diagnosis of diabetes, is becoming more common. As many as 80 million adults have prediabetes in the U.S. In addition to increasing the likelihood of developing diabetes, people with prediabetes are also more likely to suffer from a heart attack or stroke. The growing numbers of prediabetes and diabetes patients represent an immense healthcare cost, motivating researchers to learn more about this devastating and costly illness.