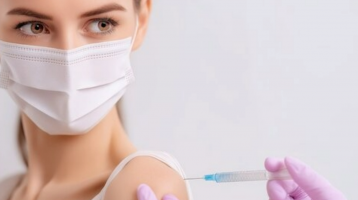
We all know how important sleep is for mental health, but a meta-analysis in the journal Current Biology found that good sleep also helps our immune system respond to a vaccine. The authors found that people who slept less than six hours a night produced significantly fewer antibodies than those who slept seven hours or more, and that this deficit corresponded to a two-month decline in antibody levels.
Less Than Six Hours of Sleep per Night Can Weaken the Immune Response to a Vaccine
“Good sleep not only enhances the vaccine’s effectiveness but can also extend the duration of vaccine protection,” said lead author Eve Van Cauter, professor emerita at the University of Chicago, who, together with first author Karine Spiegel of the French Institut national de la santé et de la médecine (INSERM), published a groundbreaking study in 2002 on the effects of sleep on vaccinations. When the COVID-19 pandemic broke out and mass vaccinations became an international priority, Spiegel and Van Cauter set out to summarize the current state of knowledge regarding the influence of sleep duration on the immune response to vaccines.
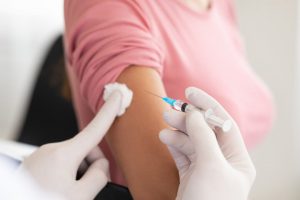
On average, people with chronic sleep deprivation produced fewer antibodies after vaccination, which may result in lower or less long-lasting protection against infection. Sleep thus appears to play an important role in activating the immune system: During sleep, inflammation-regulating signaling molecules are released, immune cells are activated, and processes necessary for the formation of a stable immunological memory are supported.
How Sleep, Hormones, and Gender Collectively Influence Vaccine Efficacy
However, a different picture emerged when the data was analyzed separately by gender: The association between short sleep duration and reduced antibody production was statistically significant primarily in men. In women, the results were significantly more variable. The researchers suspect that hormonal differences play a central role in this. Female sex hormones such as estrogen and progesterone have been shown to influence numerous immune processes. For example, estrogen can enhance certain immune responses, while progesterone tends to have a regulating or dampening effect. Since the concentrations of these hormones change over the course of the menstrual cycle, the strength of the immune response can also fluctuate.
In addition, factors such as hormonal contraception, pregnancy, menopause, or postmenopausal status can further influence the immune system. Women generally exhibit stronger immune responses to vaccinations than men, but they are also more sensitive to hormonal and physiological changes. As a result, the effects of sleep deprivation may vary more widely in women and be more difficult to clearly demonstrate in studies. The authors therefore emphasize that future research should systematically account for hormonal status to better understand gender-specific differences.
“We know from immunological studies that sex hormones influence the immune system,” explained Eve Van Cauter and her colleague Michael Irwin to Spiegel. “In women, immunity is influenced by the stage of the menstrual cycle, the use of contraceptives, as well as by menopause and postmenopausal status. Unfortunately, none of the studies we evaluated contained data on sex hormone levels.” This is precisely why the researchers see a need for further research to better understand how sleep, hormones, and gender collectively influence the effectiveness of vaccines.
Adequate Sleep as the Key to Better Vaccine Protection
Some of the studies measured sleep duration directly, either using motion-sensitive wristwatches or in a sleep lab, while others relied on self-reported sleep duration. In both cases, short sleep duration was associated with lower antibody levels, but the effect was stronger in studies that used objective sleep measurements—likely because people are notoriously bad at estimating their own sleep duration.

“If you look at the variations in protection provided by the COVID-19 vaccines—people with pre-existing conditions are less protected, men are less protected than women, and overweight people are less protected than those who are not overweight. These are all factors over which the individual has no control, but you can influence your sleep,” explained Eve Van Cauter. From the researchers’ perspective, getting enough sleep could therefore be a relatively simple and cost-effective way to support the effectiveness of vaccinations.
Many Questions Remain Unanswered
This is likely not just about the amount of sleep the night immediately before vaccination. Previous studies suggest that several nights of insufficient sleep may already be enough to alter the activity of certain immune cells. Sleep deprivation also increases the release of stress hormones such as cortisol and can influence inflammatory processes in the body. This could disrupt the communication between immune cells that is necessary to produce sufficient antibodies and memory cells after vaccination. Deep sleep in particular appears to be important for these processes, as immune-regulating signaling molecules are released in greater quantities during this sleep phase.
The researchers therefore point out that many questions remain unanswered. “We need to understand the gender-specific differences, which days around the vaccination date are most important, and exactly how much sleep is needed so that we can provide people with appropriate recommendations,” Michael Irwin told Spiegel. Future studies should therefore investigate more closely whether, for example, sleep in the days before vaccination is more important than afterward, how long the positive effect lasts, and whether targeted improvements in sleep actually have a measurable impact on vaccine protection. Equally relevant is the question of whether certain population groups—such as older adults or people with sleep disorders—might benefit particularly strongly from good sleep.